Picture this: a 68-year-old woman slips on a wet floor, breaks her hip, and is diagnosed with osteoporosis. Her doctor calls it an “age-related condition.” Her family assumes it crept up in her 60s. But here’s the truth, that fracture has been 40 years in the making.
Osteoporosis isn’t a disease that arrives with old age. It’s a disease that reveals itself in old age, long after the real damage was done.
The Silent Thief That Starts in Your 30s.
Here’s the number that should stop you mid-scroll.
Women and men alike begin losing bone in their mid-30s (Osteoporosis Canada, 2022). Not their 50s. Not after menopause. Their mid-30s, often when people feel strongest, most active, and least concerned about skeletal health.
From 20-35, or maybe even 40, our peak bone mass is achieved and then starts to decline over many years until we experience significant bone loss after menopause (2-4% per year for the first 10 years post-menopause). Many women experience this accelerated bone loss around the same time they start experiencing menopauses.
Osteoporosis is often diagnosed long after significant structural damage has already occurred. The recent 2024 Korean Society of Menopause Guidelines claim that individuals who do not achieve peak bone mass during childhood or adolescence may be at risk for developing osteoporosis at any point after the age of 50 regardless of whether they have experienced menopause and/or age-related changes.
In addition, the stakes are extremely high as fractures due to osteoporosis occur more frequently than heart attacks, strokes, or breast cancer combined. In fact, 22% of women and 33% of men will die within one year of having a hip-related fracture. This statistic is about decades of bone loss, not age.
Why Bone Loss Goes Undetected for Decades?
Osteoporosis is known as the “silent thief” for a reason. There are no symptoms. No painful bones, no noticeable symptoms, no blood test to detect it early. Most people don’t know they have low bone mass until a bone break occurs.
What makes this so tragic is that the underlying biology of bone loss begins subtly and adds up over the years. Poor skeletal nutrition in young people leads to failure to reach genetically determined peak bone mass, while in middle-aged individuals, it leads to the rapid loss of bone mass that triggers or exacerbates osteoporosis (PMC, 2017). By the time it appears on the imaging study, you’re late. You’re late.
How Terraquino’s K2-7 Defends Bone Over the Long Term?
This is precisely where long-term K2-7 supplementation becomes a defining strategy and not a quick fix, but a sustained, lifelong defense.
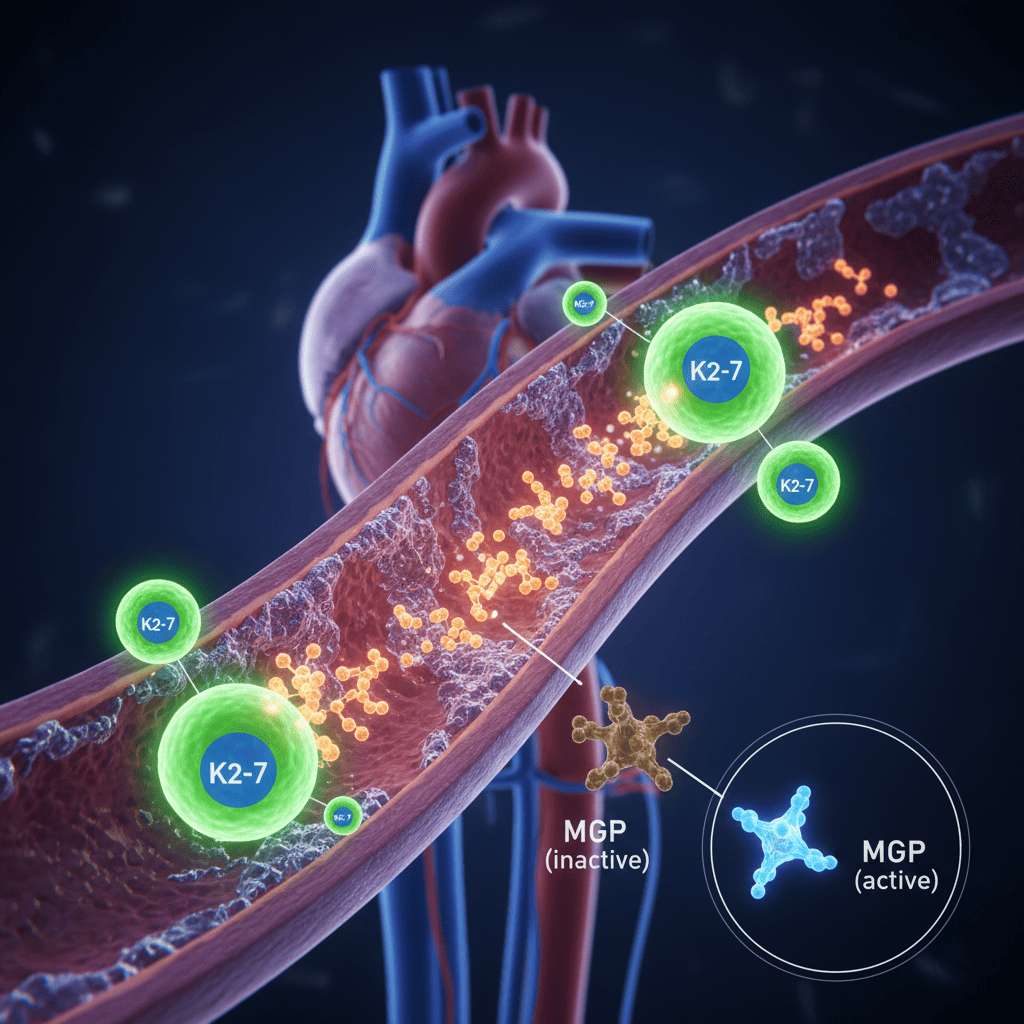
Vitamin K2 is an important part of the carboxylation process for osteocalcin, the protein that connects calcium to bone mineral matrix and promotes both mineralization and strength of bone. Without vitamin K2 present, osteocalcin is inactive (circulating), meaning that any calcium consumed cannot be utilized by the bones (PubMed, 2021).
The evidence supporting K2-7 is substantial in terms of its clinical effectiveness. A landmark 3-year randomized, placebo-controlled study noted that postmenopausal women taking 180 mcg/day of vitamin K2-7 (known as MK-7) experienced significantly less decrease in both bone mineral density and bone strength associated with age than did the placebo group (PubMed, 2013). In a different 3-year randomized study of postmenopausal women, the MK-7 group experienced a 65.2% decrease in their undercarboxylated osteocalcin levels compared to no change in the undercarboxylated osteocalcin levels of women in the placebo group (Osteoporosis International, 2021).
There was a comprehensive meta-analysis of 16 randomized controlled trials (RCTs) with 6,425 total subjects that demonstrated that vitamin K2 supplementation results in significant increases in lumbar spine bone mineral density (BMD) and decreases the incidence of fractures in postmenopausal women (Frontiers in Public Health, 2022). In addition, there is evidence that vitamin K2 has a synergistic effect when administered with vitamin D3 and calcium; the combined vitamin K2, vitamin D3, and calcium has significantly better outcomes for bone mass compared to the individual interventions alone (PMC, 2017).
Terraquino’s K2-7 delivers Menaquinone-7, the form with the longest half-life and greatest bioavailability for bone tissue ensuring that osteocalcin stays activated, calcium gets directed into your skeleton, and bone remodeling remains in healthy balance year after year.
The Best Time to Start Is Before You Need To.
One in three women and one in five men will experience an osteoporotic fracture in their lifetime (Osteoporosis Canada, 2022). Most of them never saw it coming, because bone loss gave them no reason to look.
You don’t wait for a house fire to install smoke detectors. You shouldn’t wait for a fracture to protect your bones.
At Terraquino, we believe skeletal health isn’t a concern for your 60s, it’s a commitment that starts today. Our K2-7 supplement supports long-term bone mineral density, activates the proteins your skeleton depends on, and ensures the foundation you’re living in stays strong decade after decade.
The fracture at 68 was preventable. It just needed to be addressed at 38.